About Histopathology
Histopathology is concerned with the morphological study of the effect of disease on cells or tissues of the body. This study can take the form of one of three types of activity:
· Histology
· Cytology
· Autopsy
The job of the histopathologist is to integrate clinical information with the macroscopic and microscopic appearance of tissues to answer questions posed by the clinicians. These questions will generally relate to diagnosis, treatment or prognosis. It is therefore essential that the histopathologist knows the parameters that will affect these decisions and spends the finite time and resources available to provide this key information. Opinions are communicated by constructing written reports; all histopathology reports have the same basic structure:
· Macroscopic description
· Microscopic description
· Conclusion/diagnosis
The role the histopathologist plays in determining patient management is best evidenced by their participation as key members of the Multi-Disciplinary Team. Attendance at these meeting is extremely useful and helps to reinforce the key information to be included in reports.
Histology
Histology forms approximately 90% of the workload of most general Consultant Histopathologists. 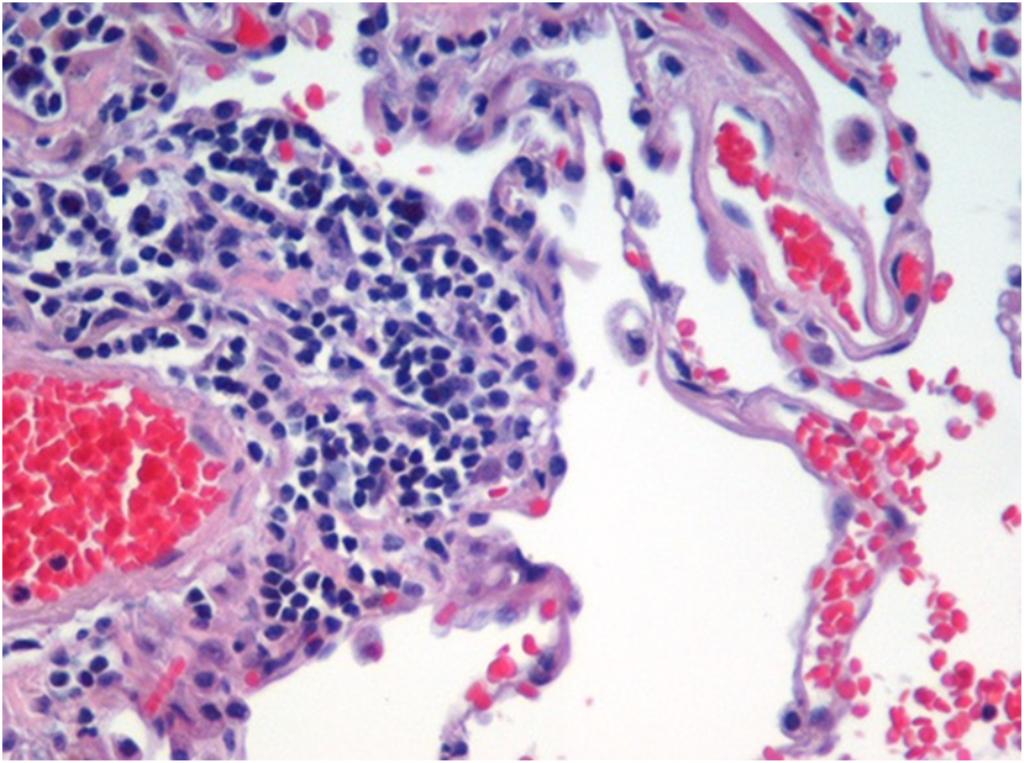 The specimens are generally either biopsies or resection specimens. Biopsies are processed by biomedical scientists in the laboratory, whereas resection specimens are usually ‘trimmed’ by consultants or trainees, according to standardised guidelines. For example, a specimen e.g. mastectomy, is booked in and taken to the cut-up room. The specimen is opened to allow optimal fixation by formalin. The specimen is next examined and slices of tissue placed in cassettes. The tissue is processed, embedded in paraffin wax and sections cut and placed onto glass slides. The case is then examined under the microscope and if required various special stains or immunohistochemical tests requested. Finally a report is written conveying the findings.
The specimens are generally either biopsies or resection specimens. Biopsies are processed by biomedical scientists in the laboratory, whereas resection specimens are usually ‘trimmed’ by consultants or trainees, according to standardised guidelines. For example, a specimen e.g. mastectomy, is booked in and taken to the cut-up room. The specimen is opened to allow optimal fixation by formalin. The specimen is next examined and slices of tissue placed in cassettes. The tissue is processed, embedded in paraffin wax and sections cut and placed onto glass slides. The case is then examined under the microscope and if required various special stains or immunohistochemical tests requested. Finally a report is written conveying the findings.
In certain circumstances the surgical team may want to send tissue straight from theatre to the pathology lab for immediate assessment. The tissue is frozen allowing sections to be taken straight away with a microtome. Following microscopic assessment findings are phoned through to the surgeon.
Cytology
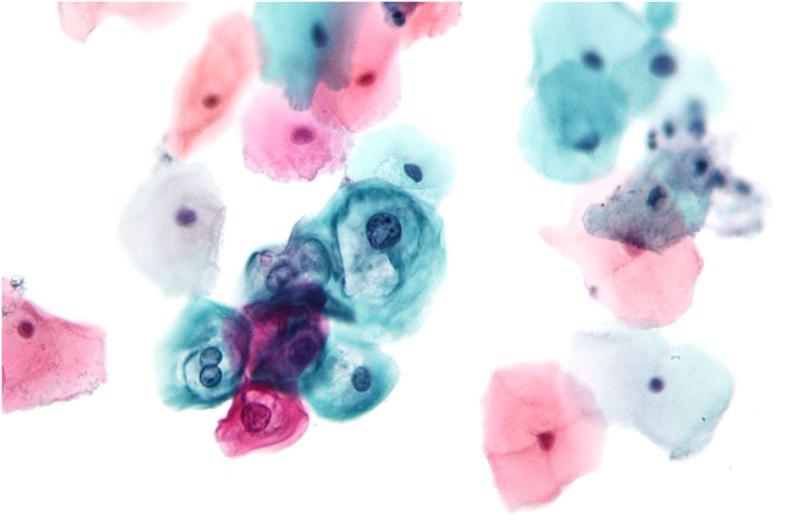 Cytology is the study of morphological characteristics of individual cells. The subject is divided into two key areas:
Cytology is the study of morphological characteristics of individual cells. The subject is divided into two key areas:
· Cervical cytology: This branch of cytology is concerned with the interpretation of cervical smear cytology and is thus linked to the national cervical cancer screening programme.
· Non-Gynaecolgical Cytology: This branch of cytology is concerned with the interpretation of all other cytology specimens e.g. ascitic fluid or pleural fluid.
Autopsy
There are three types of post-mortem:
· Hospital post-mortems: These are now few and far between. They are cases in which the cause of death is known, but the medical team have requested a post-mortem to answer specific questions. Consent is required and the examination may be limited. There may also be limitations on samples the pathologist is permitted to take.
· Coroners post-mortems: The majority of post-mortems trainees perform are of this type. There are a number of situations when a death must be reported to the coroner. The coroner may request a post-mortem to answer a particular question, for example, what is the cause of death. A report is issued to the coroner and the pathologist may have to discuss the findings at inquest.
· Forensic post-mortems: These are performed by a home office registered pathologists when there are suspicious circumstances surrounding a death.
Specialty Attractions
· Lab based specialty different from other specialities
· A cerebral speciality with a wide range of interesting pathologies
· Opportunities for subspecialisation
· Close working with the multi-disciplinary team
· New molecular and immunological techniques make it a cutting edge speciality
· Ample opportunity for teaching and research
· Largely routine working hours with little on-call
· Although patient contact is generally very limited, opportunities do exist
Personal qualities include:
· Interpretative, analytical and critical thinking
· Good problem-solving and decision-making
· Enjoy working as part of a team
· Good written and verbal communication skills
· Williningess to engage in life long learning
· Exceptional attention to detail
· A degree of manual dexterity
Website Updated 08.07.2021